Alberta Family Integrated Care (FICare™) in Level II NICUs
Family Integrated Care (FICare™) in Level II NICUs: An Innovative Program for Alberta
In Alberta, one in every 12 babies is born preterm (more than 3 weeks early). Parents must leave their preterm babies in the neonatal intensive care unit (NICU) to fully develop enough to care for them at home. When it is time for discharge, parents are often unprepared to look after their baby because they may have limited involvement in the care of their baby in hospital. The purpose of this project is to test a new way to integrate and involve parents into the care of their baby through a program called Alberta Family Integrated Care (FICare™). Alberta FICare™ provides tools and strategies to empower parents to build their knowledge, skill, and confidence to ensure they’re well-prepared to care for their preterm infant before going home.
Alberta FICare™ consists of:
- Relational Communication
- Parent Education
- Parent Support
Alberta FICare™ was tested in 10 level II NICUs in Alberta with babies born 6 – 8 weeks early. The purpose of this study was to examine if Alberta FICare™ decreased the infant length of stay in hospital, and other baby and mom outcomes such as maternal mental health, infant growth and development, and family perceptions of Alberta FICare™. If Alberta FICare™ contributes to positive outcomes for parents and families, then it will be sustainably implemented in all Alberta NICUs.
Click HERE to discover how your NICU can adopt this positive practice change.
Study Status: Completed

Principal Investigator: Karen Benzies RN, PhD
Co-Investigators:
Khalid Aziz MBBS, MA, MEd (IT), FRCPC, FRCPCH, FAAP
Vibhuti Shah MD, DCH, MBBS, MRCP, FRCPC
Abhay Lodha MBBS, MD, DM, MSc
Collaborators:
Harish Amin MD
Radha Chari MD
Kelly Mrklas PhD(c)
Jeffrey S. Hoch MD, PhD
Christopher Naugler MD, CCFP, FCFP, FRCPC
Tom Stelfox MD, FRCPC, PhD
Esther Suter PhD, MSW
Jill Larcoque NNP
Jeanne Scotland NNP
Sandra Walker-Kendall NNP
Alberta FICare™ reduced infant hospital length of stay by 2.55 days, without a concomitant increase in readmissions or emergency department visits. Read the clinical trial results published in BMC Paediatrics. Click HERE to discover how your NICU can adopt this positive practice change.
Implementation of family-centred care initiatives is often challenging due to a poor understanding of contextual factors of the implementing organization. We identified many facilitators to implementation of Alberta FICare™ including (1) the capacity for change, (2) compatibility of Alberta FICare™ with existing family centred care practices, (3) available resources and access to knowledge for neonatal care providers, (4) engagement of key stakeholders at all levels of the organization, including families, and (5) evaluation. Notable barriers included the design and delivery of staff training, relative priority against competing initiatives, and the learning climate of the implementing organization. Future implementation of Alberta FICare™ should be purposefully planned to assess and manage the influence of contextual factors.
Additional study data is currently being analyzed and results will be shared as they become available.
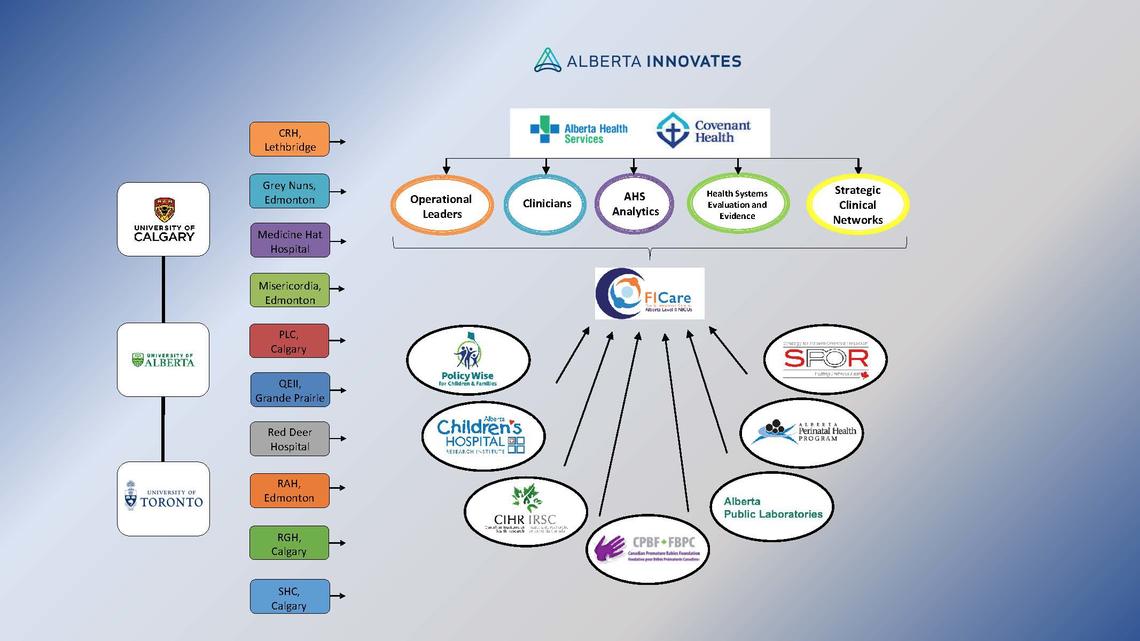
Sponsors and Partners
The Benzies Lab would like to acknowledge funding from Alberta Innovates Partnership for Research and Innovation in the Health System (PRIHS) Program and support from our valued partners;
- University of Calgary
- University of Alberta
- University of Toronto
- Alberta Health Services (AHS)
- Covenant Health
- Alberta Innovates Strategy for Patient-Oriented Research (SPOR)
- Alberta Perinatal Health Program
- Alberta Public Laboratories
- Canadian Premature Babies Foundation
- Canadian Institutes of Health Research (CIHR)
- Alberta Children's Hospital Research Institute (ACHRI)
- Policy Wise for Children and Families